Schools
Maryland Schools Required to Carry Epinephrine Injectors, But is it Safe?
An Upper Marlboro doctor discusses how schools prepare to safeguard students with allergies.
Q: I just heard that there are some states that require public schools to have epinephrine injectors not targeted for a specific child available in case of an emergency. Is this safe?
- Sydney, Crofton
A: This is a perfect topic to discuss as Food Allergy Research & Education (FARE)’s Food Allergy Awareness Week, was last week. What you are referring to is called the “stock” epinephrine law, which has been enacted by about 20 states thus far, including Maryland and Virginia. It requires schools to keep epinephrine stocked for use in case of an emergency for children who do not have their own prescription epinephrine injectors at the school.
Find out what's happening in Upper Marlborowith free, real-time updates from Patch.
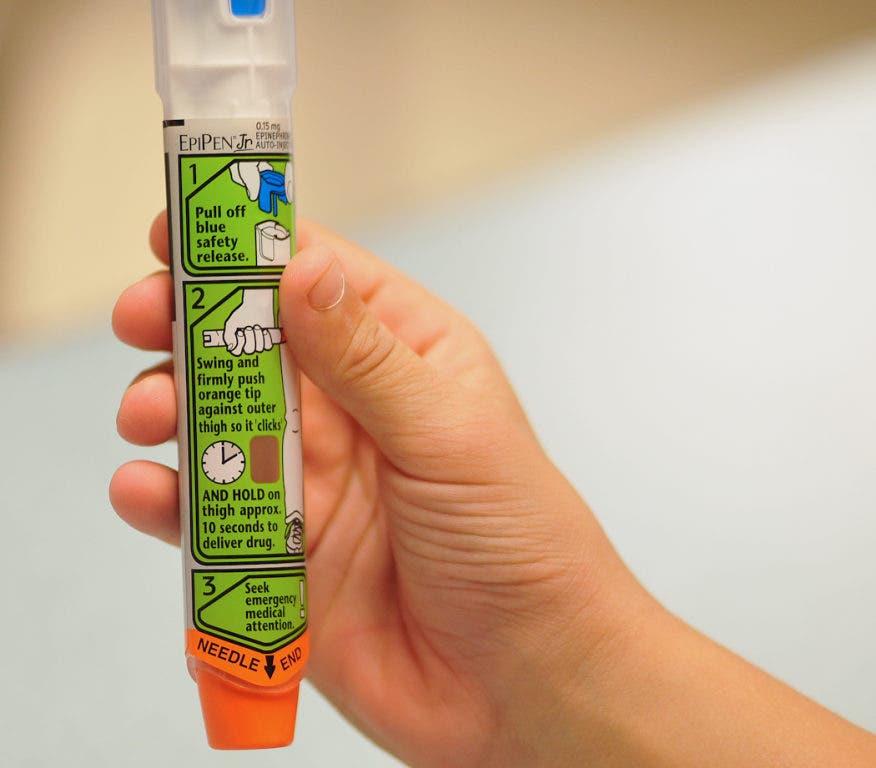
When someone comes into contact with a food allergen, an immune response is triggered and anaphylaxis may occur. Anaphylaxis is a serious life-threatening medical condition if not treated properly. Epinephrine (otherwise known as adrenaline) is the first-line medication indicated for anaphylaxis and is nearly always effective if given immediately. Delay increases the risk of a poor outcome and even fatalities. In fact, if one suspects a severe allergic reaction, it is better to give an epinephrine injection, even if it turns out to be an unnecessary dose, as the most common risk is a temporary increased heart rate. In a nutshell, it is considered a safe medication that saves lives. There are currently three auto-injectors on the market, Epi-pen, Auvi-Q and Twin-ject, and there are only two doses – for those under 30kg and over 30kg.
Every classroom has, on average, two students with food allergies. There have been deaths in schools where allergic students either did not have their own epinephrine accessible during an emergency, or the student had their first severe allergic reaction while at school. Approximately 20-25% of students or staff members who may need epinephrine in school do not have a history of food, bee sting, latex or other allergy, and therefore would not have their own prescription.
Find out what's happening in Upper Marlborowith free, real-time updates from Patch.
Only last year, in Virginia, first-grader Amarria Johnson tragically died from an anaphylactic reaction at her school last year after eating a peanut. Epinephrine was not given, though several other students’ injectors of the same dose were available. If the law was in place, it may have saved her life. As a result, the now-passed law in Virginia is called Amarria’s law.
In some cases, only a school nurse can administer the epinephrine, while in others, other trained personnel may administer the medication in an emergency. For those students who have already been diagnosed with allergies and have their own epinephrine at school, schools will still give them their own epinephrine. However, the new law adds an extra level of safety since these students will have a backup device at school in case their own injector is lost or expired. In addition, the law addresses liability concerns for those who administer the medication in good-faith.
Last week, I attended a congressional briefing on Capitol Hill where we demonstrated that evidence-based anaphylaxis care saves lives and money. The stock epinephrine law is one safe, effective means to protect the growing number of children with life-threatening allergies. Schools are meant to bee safe places for children; access to epinephrine via this law helps ensure this.
Just some food for thought!
- Dr. Sharif